The historic decision could revolutionize the treatment of sickle cell disease and -thalassaemia, but the technology is too pricey.
The UK medicines regulator has approved a new therapy that uses CRISPR gene editing to treat sickle-cell disease and beta-thalassemia. This is the first time that CRISPR has been approved for use in humans.
The therapy, called Casgevy, is a one-time treatment that involves taking a patient’s blood stem cells, editing them with CRISPR, and then putting them back into the patient’s body. The edited cells produce fetal hemoglobin, which is a type of hemoglobin that does not cause the symptoms of sickle-cell disease or beta-thalassemia.
Studies have shown that Casgevy is very effective at treating both sickle-cell disease and beta-thalassemia. In one study, 28 of 29 patients with sickle-cell disease who were treated with Casgevy did not have any pain crises for at least one year. In another study, 39 of 42 patients with beta-thalassemia who were treated with Casgevy did not need any blood transfusions for at least one year.
Casgevy is a very expensive treatment, with an estimated cost of around US$2 million per patient. However, it is a major step forward for the treatment of sickle-cell disease and beta-thalassemia.
How does Casgevy work?
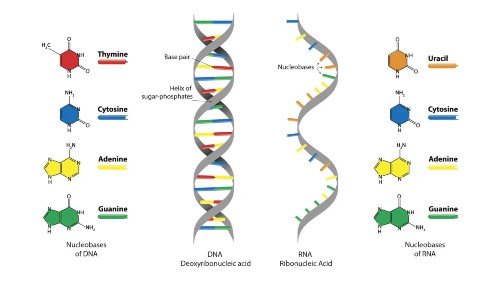
Casgevy relies on the gene-editing tool CRISPR, the developers of which won the Nobel Prize in Chemistry in 2020. Sickle-cell disease and beta-thalassemia are caused by errors in the DNA sequence of genes that encode for haemoglobin, a molecule that helps red blood cells to carry oxygen around the body.
In sickle-cell disease, abnormal haemoglobin makes blood cells misshapen and sticky, causing them to form clumps that can clog blood vessels. These blockages reduce the oxygen supply to tissues, which can cause periods of severe pain, known as pain crises.
Beta-thalassaemia occurs when mutations in the haemoglobin gene lead to deficient or absent levels of the oxygen-carrying molecule in red blood cells, low numbers of red blood cells and symptoms such as fatigue, shortness of breath and irregular heartbeats.
Clinicians administer Casgevy by taking blood-producing stem cells out of the bone marrow of people with either disease and using CRISPR to edit genes encoding for haemoglobin in these cells. The gene-editing tool an RNA molecule that guides the enzyme to the correct region of DNA and a Cas9 enzyme that cuts DNA.
Once the Cas9 enzyme reaches the gene targeted by Casgevy, called BCL11A, it cuts both DNA strands. BCL11A usually prevents the production of a form of haemoglobin that is made only in fetuses. By disrupting the BCL11A gene, Casgevy unleashes the production of fetal haemoglobin, which does not carry the same abnormalities as adult haemoglobin in people with sickle cell or beta-thalassemia patients.
Before the gene-edited cells are infused back into the body, people must undergo a treatment that prepares the bone marrow to receive the edited cells. Once administered, the stem cells give rise to red blood cells containing fetal haemoglobin. After some time, this relieves symptoms by boosting the oxygen supply to tissues. “Patients may need to spend at least a month in a hospital facility while the treated cells take up residence in the bone marrow and start to make red blood cells with the stable form of haemoglobin,” the MHRA said in a press release.
How safe is Casgevy?
Participants involved in the trials, which are ongoing, experienced side effects including nausea, fatigue, fever and an increased risk of infection, but no significant safety concerns were identified. The MHRA and manufacturer are monitoring the safety of the technology and will release further results.
One concern surrounding the approach is that CRISPR can sometimes make unintended genetic modifications with unknown side effects.
“It is well known that CRISPR can result in spurious genetic modifications with unknown consequences to the treated cells,” geneticist David Rueda at Imperial College London told the SMC. “It would be essential to see the whole-genome sequencing data for these cells before coming to a conclusion. Nonetheless, this announcement makes me feel cautiously optimistic.”
When will Casgevy be available?
The US Food and Drug Administration is considering approval of Casgevy, whose generic name is exa-cel, for sickle-cell disease; its advisers met last month to discuss the therapy. The European Medicines Agency is also reviewing the treatment for both diseases.
For now, the therapy is likely to remain the reserve of rich nations with developed health-care systems. “This treatment may not easily scale up to be able to provide treatments in low- and middle-income countries, since it requires the technology to obtain a patient’s blood stem cells, deliver

